Patient-Centric Remote Cardiac Monitoring: Device Options, and How Long is Enough?
- David Bragg, MD

- Jan 23, 2022
- 3 min read
Updated: Jan 23, 2022
You’re a typical patient, relatively healthy, and check your blood pressure at the drug store periodically. Recently, you noticed that sometimes your heartbeat is irregular when checking your blood pressure, yet you feel fine. You repeatedly tell yourself that it’s nothing to worry about. However, you secretly worry. You begin your own internet research and quickly learn that some cardiac arrhythmias can lead to fainting, strokes, and even sudden death. You finally decide to see your doctor to check it out.
Scenario 1- You see your PCP who examines you, does an EKG which is normal, then you’re referred to a Cardiologist for further evaluation. The Cardiologist “squeezes you in” 2 weeks later and orders a 24 Holter monitor. 10 days later (average result notification time) they inform you that the Holter is normal, and they order a 30-day Event monitor. 5 weeks later you are notified that this too, was normal. You are frustrated, and still have no answers.
Total evaluation time: 8 ½ weeks with no diagnosis.
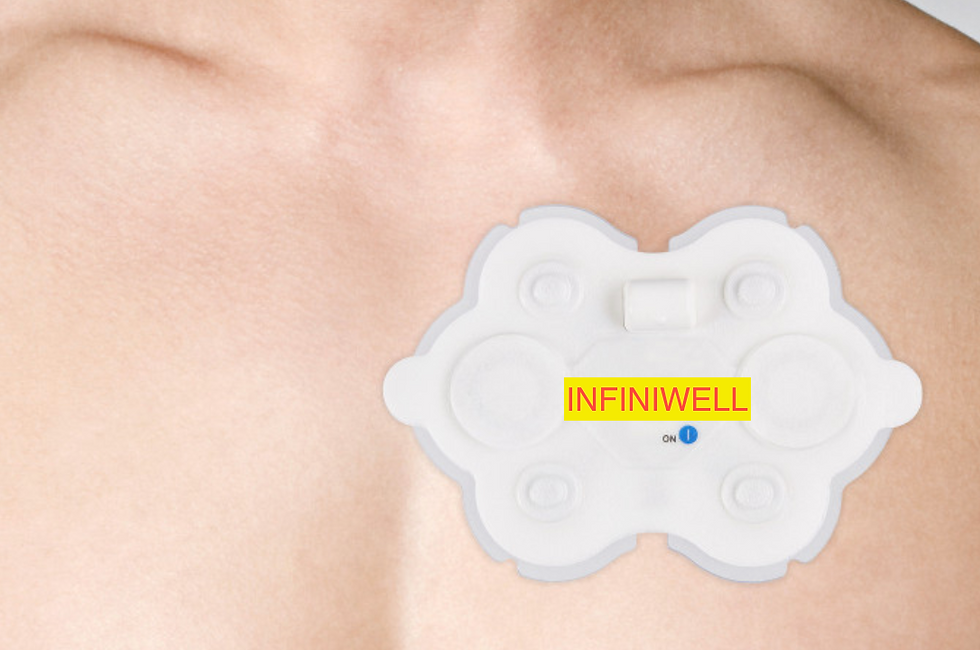
Scenario 2- You see your PCP who examines you, does an EKG which is normal, then applies a wireless patch to your chest and sends you home with active monitoring of your heart for the next 10 days. You receive results 24 hours after completion of the monitoring with a harmless diagnosis. You’re advised to reduce caffeine and given much reassurance.
Total evaluation time: 11 days with diagnosis and treatment recommendations.
Unfortunately, scenario 1 is the “norm” in today’s medical climate.
Background: Cardiac arrhythmias are very common, but frequently go undiagnosed due to the transient and often asymptomatic nature of the condition. Atrial fibrillation (AFIB), for example, is often asymptomatic, and is associated with serious sequelae such as stroke and death. The management of AFIB alone costs between $25-$30 B annually. Since proper diagnosis and treatment can reduce both morbidity and mortality of certain arrhythmias, identifying arrhythmias is critical. However, this is often easier said than done.
Traditionally, physicians have been taught to follow a sequence when evaluating a patient for cardiac arrhythmias. The initial test is usually a standard 12 lead ECG, which has an extremely low yield in establishing the problem. The next step traditionally recommended is a 24-hour Holter monitor. Besides the multiple issues with the standard Holter monitor (cost, cumbersome wires, size, etc.), the yield rate of identifying the arrhythmia is quite low, generally between 15%-35%. (Note- one study revealed that 76% of patients stated the Holter monitor interfered with their daily activities).
The next step traditionally recommended is either to repeat the 24-hour Holter, or to use an “event recorder” for 30 days to months. While the diagnostic yield does often increase using an event recorder (if the patient is symptomatic), it too has its own issues. The total cost is typically around $1,000 or more, and one must avoid metal detectors, microwave ovens, garage door openers, electric blankets, etc. Additionally, about 1 in 4 patients are unable to activate the recorder in a timely manner to capture the arrhythmia. Obviously, if the patient has no symptoms, then the likelihood of capturing the arrhythmia is unlikely.
This begs the question, isn’t there a better way? Fortunately, the answer is yes. Multiple studies have shown that continuous monitoring for a period of 10-14 days delivers the maximum diagnostic yield (range of diagnostic yield %60-%90). In other words, this is the sweet spot for ambulatory cardiac monitoring.
The final key point, monitor type, is just as crucial as length of monitoring time. Disposable, wireless cardiac patches are more effective than traditional bulky hardware monitors when it comes to detecting cardiac arrhythmias. Not only are these patches wireless, most are water resistant, less expensive, can be monitored in real-time, and they also allow the user to go about their normal lifestyle. One study showed that 81% of patients preferred wearing a cardiac patch over using a Holter monitor. Unfortunately, most physicians have not yet adopted the use of these wireless, wearable cardiac patches.
Isn’t it time that we adopt the evidence based, patient-centric modes of remote cardiac monitoring? As a patient, which would you prefer, scenario 1 or 2?
For more information about patient-centric Cardiac monitoring options offered by Infiniwell, please contact us.
David Bragg, MD
CMO Infiniwell.ai


Comments